
Etiology: the retina splits in the nerve fiber layer, similar to Juvenile X linked retinoschisis.Appearance: an oval shaped, bullous elevation with a finely stippled internal surface and sclerotic looking retinal vessels typically located posterior to and continuous with typical peripheral cystoid degeneration.Thus the risk for retinal detachment is lower than that of the reticular subtype Complications: it is very uncommon for the retinal splitting to extend posteriorly towards the macula or form outer layer holes.Etiology: the retina splits in the outer plexiform layer, allowing the visualization of the footplates of the Muller cells, seen as white dots.Appearance: a bubbly, round appearance best visualized with scleral depression the retinal splitting typically extends 2-3mm posterior to the ora.Two histological forms, typical and reticular, have been previously described. This produces a well-circumscribed, transparent dome-shaped elevation of the inner retina that extends anteriorly towards the ora serrata. Acquired retinoschisis, also known as degenerative or senile retinoschisis, is an acquired, idiopathic condition characterized by gradual, peripheral splitting of retinal layers. Retinoschisis (RS) literally means "a split in the neurosensory retina". Minimal pigment alterations or atrophy of the retinal pigment epithelium layer.The lesion appears relatively immobile, transparent, smooth-domed and bullous in appearance. Elevation of the inner layers of the neurosensory retina due to microcystoid degeneration.DIAGNOSIS Acquired retinoschisis Diagnostic Criteria 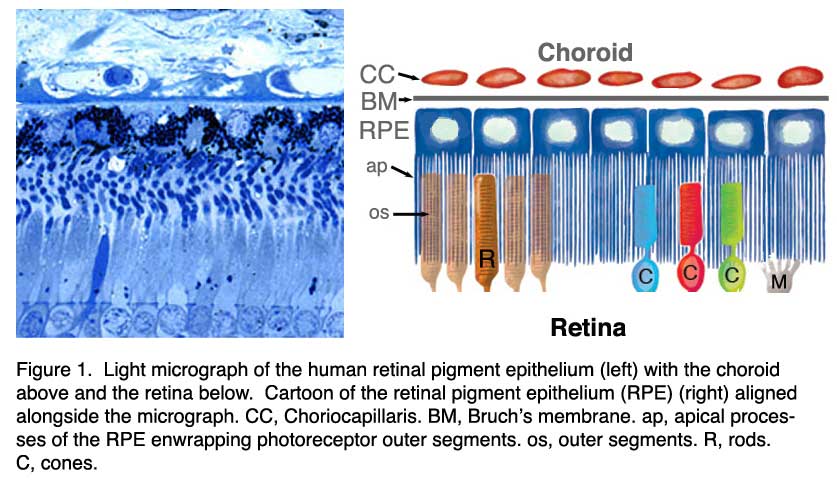
Signs and symptoms of retinal detachment were reviewed and he was provided with reassurance. No ophthalmologic intervention was necessary. The patient underwent an uncomplicated clinical course. Periphery shows a faint shallow retinoschisis inferotemporally for 4-5 clock hours, much less bullous compared to the right eye.Vitreous: No PVD, no heme or pigment, no vitreous cells.There is an absolute visual field deficit through the entire area.įigure 1a: (OD) Fundus photo showing temporal retinoschisis from 7:00 to 10:00 without identified inner, outer, or full-thickness retinal breaks extending into the temporal macula.įigure 1b: Here is an additional picture of a different patient showing inferotemporal retinoschisis Periphery: Temporal retinoschisis from 7:00 to 10:00 without identified inner, outer, or full-thickness breaks inferior edge adjacent to area of chorioretinal atrophy.Vitreous: No posterior vitreous detachment (PVD), no heme or pigment, no vitreous cells.Lens: 2+ nuclear sclerosis, 1+ posterior subcapsular cataract.OD: Partial superior temporal, inferior temporal deficiencies. 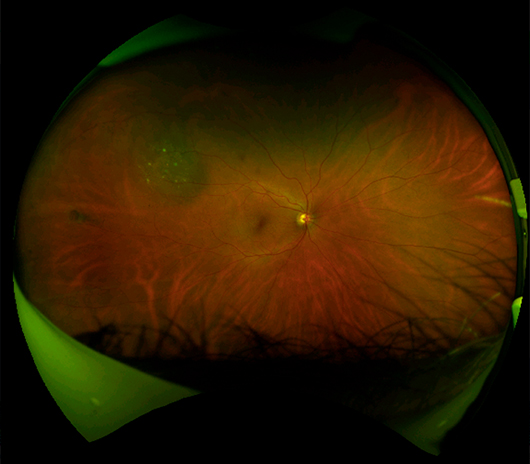
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
